
|
|
Research HighlightHelping Veterans Quit the Expanding Continuum of Tobacco ProductsKey Points
Tobacco use remains the number one cause of mortality and morbidity among adults in the United States and contributes to more than 480,000 deaths every year. Tobacco use among Veterans remains higher than in the non-Veteran U.S. population, with 21.6 percent of Veterans reporting current cigarette use and 29.2 percent reporting current use of any tobacco product.1 Veterans with Posttraumatic Stress Disorder (PTSD), a prevalent mental health disorder among Veterans, have a more complicated path to quitting as evidenced by lower quit rates than those of Veterans without PTSD. Smoking continues to contribute to high morbidity and mortality rates among Veterans receiving care at the Veterans Health Administration (VHA). In the VHA alone, tobacco-related conditions are estimated to cost approximately $2.7 billion.1 We tested the effectiveness of a home telehealth care management program on smoking cessation rates in 175 Veterans with PTSD enrolled in the Eastern Colorado Health Care System in a two-arm study.2 Both arms received the PTSD home telehealth care management program, which was designed to help Veterans with PTSD self-monitor and self-manage. Both groups also had access to smoking cessation treatments offered by VHA, such as medications, tobacco cessation clinic, support groups, and classes. We designed the intervention to take place over 12 weeks, with daily sessions over 90 days, and we followed Veterans for six months after the intervention ended. Veterans had the option of continuing to use the PTSD home telemonitoring system during the follow-up period. This pragmatic randomized controlled study did not show a significant difference in 24-hour quit attempts, seven-day point prevalence, or progression along the stages of change. Favorable smoking cessation rates were seen in both groups without negatively impacting PTSD symptoms and suicidal ideations. Depression symptoms improved in the intervention group during intervention and follow-up periods. Rise in Use of Alternative Forms of TobaccoAs cigarette smoking declines, alternative forms of tobacco use, such as electronic nicotine delivery devices (e-cigarettes) and waterpipes, are on the rise. The current literature on the use of these tobacco products is limited. We used data from The Attitudes and Behaviors Survey (TABS) on Health conducted in 20153 to investigate the prevalence of different forms of tobacco use among adults in Colorado. Results showed a lifetime prevalence of cigarette-only use was 25.8 percent, compared to 10.8 percent ever waterpipe use, 7 percent for dual users (traditional and e-cigarettes), and 12.6 percent for anything else (any tobacco product except cigarettes). Based on the TABS data, we wanted to learn about Veterans’ experiences with a variety of tobacco products. We conducted a survey among Veterans seeking care at the Rocky Mountain Regional VA Medical Center to learn about their use, perceptions, and knowledge of the hazards linked to alternative tobacco products.1 Of the 200 respondents, 76 percent had ever tried cigarettes, 63 percent were lifetime cigarette smokers (smoked more than 100 cigarettes in their lifetime), 23.5 percent were current daily cigarette smokers, and 12.5 percent smoked on some days during the week. Fifteen percent of respondents reported ever vaping, and 13 percent reported ever using a waterpipe. Results revealed that 1 percent of the respondents were current waterpipe users while 2 percent were current vape users. Among those reporting ever using cigarettes, 27.5 percent reported ever vaping and/or using waterpipe. Among those reporting ever using cigarettes, 27.5 percent reported ever vaping and/or using waterpipe. Although 40 percent of respondents stated both vaping and waterpipe were very harmful, 42.5 percent of respondents did not know the level of harm from waterpipe use. Moreover, 12.5 percent of respondents believed vaping would help them quit using cigarettes. Cessation efforts in VA have primarily focused on more traditional forms of tobacco use such as cigarettes, cigars, pipes, and chewing tobacco. According to VA Directive 1056, the VA provides a Smoking and Tobacco Use Cessation Program that delivers care according to the U.S. Preventive Services Task Force and the U.S. Public Health Service Clinical Practice Guidelines. VA Directive 1056 requires primary and other clinical care settings to provide brief counseling and smoking cessation medications to all Veterans interested in quitting smoking, regardless of whether they attend a tobacco use treatment program. In accordance with current VA and non-VA quality of care measures for tobacco use treatment, all Veterans are screened for current tobacco use; current tobacco users receive advice to quit and are offered behavioral counseling and medications. However, standard reminders may not capture all the different forms of tobacco use that are prevalent today among younger Veterans. Focus Cessation on Alternative Tobacco ProductsGiven all of the efforts to reduce traditional forms of tobacco use, it is time to focus our cessation efforts on alternative forms of tobacco. These forms of tobacco are not approved by the FDA to help in tobacco cessation, despite some users’ perception. There are no specific guidelines to assist patients who want to quit these types of tobacco use. The literature lacks adequate information on the use of vaping and other alternative tobacco products among Veterans and the science on the hazards of vaping and alternative tobacco products is not conclusive, though there is evidence that these products might be gateway drugs to cigarette use. The Centers for Disease Control and Prevention is investigating the association between vaping and lung disease. Future research should investigate the prevalence and specific health hazards of alternative forms of tobacco use among Veterans. We plan to conduct an educational awareness campaign aimed at stopping the use of these alternative forms of tobacco. 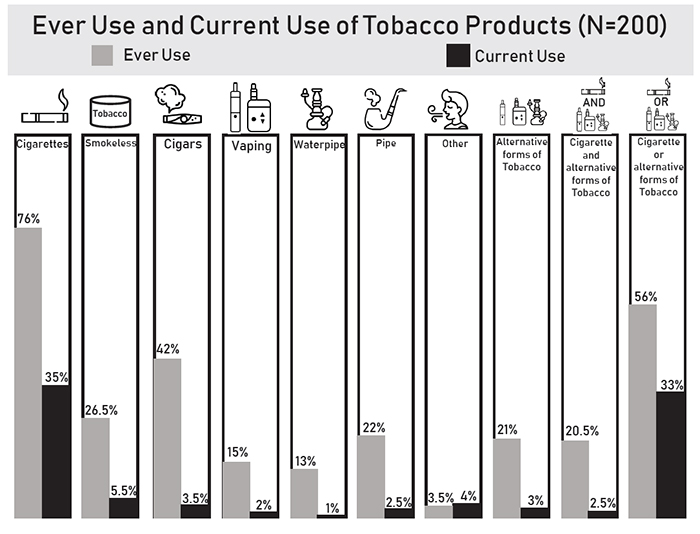
References
|
|