
|
|
Response to CommentaryTumultuous Times Require Novel Tools and Partnerships to Maintain Patient Satisfaction and TrustThe Veterans Experience Office (VEO) is a critical and innovation-driven arm of the Department of Veterans Affairs (VA) that is tasked with improving the experience of care for our Veteran customers. As Richardson and colleagues demonstrate, the VEO has developed a suite of tools to address Veteran needs. The Office comprehensively targets experiences across the lifecycle of Veteran experience within VA, including families and caregivers, and looks at the range of VA benefits. The VEO also integrates stakeholder engagement using its Veteran, Family, and Community Engagement Office, which partners with thousands of community groups in a grass-roots network. Importantly, the VEO emphasizes the need to innovate, representing experiences from an initial appointment to service delivery, drawing upon both quantitative and qualitative data. Many healthcare systems focus on measuring patient experience and satisfaction with standardized surveys. VA has used the Survey of Healthcare Experiences of Patients (SHEP) for many years to track facility performance on patient experience metrics. The VEO adds a novel approach, capturing real-time satisfaction data through their Veterans Signals (VSignals) electronic tool, which is tied to specific visits. Importantly, it also encourages comments with opened-ended questions. The analysis of such narratives relies on artificial intelligence, providing complex feedback at a scale and within a timeframe that further improves the VA system’s responsiveness to its customer needs. The VEO’s analysis of Veteran experience data identifies areas in need of improvement. The design of their tool also drives changes across the entire spectrum of VA services. Moreover, the VEO seeks to achieve high satisfaction equitably across VA medical centers by applying their Five Foundational VA PX Tools. Our own data from the Disparities In Satisfaction with [VA] Care (DISC) study highlights the need for such tools, as we found substantial differences in Veteran satisfaction with care across VA facilities.1 It is promising that the VEO is now focused on COVID-19. VA will need to ensure a positive patient experience both during and after the pandemic. Our research shows the impact that transitions and disruptions can have on satisfaction and trust in VA. In our work on the early rollout of the Veterans Choice Program, we found substantial barriers and dissatisfaction with Choice during the early implementation, demonstrating the importance of system stability during times of change.2 Similarly, our DISC study captured the natural experiment of the access “scandal” that occurred on April 23, 2014, when CNN first reported on the hidden waitlist at the Phoenix VA. Because our DISC interviews included a validated measure of Health System Distrust, we were able to correlate the timing of news coverage with increases in Veteran distrust. As shown in Figure 1, we found small increases in distrust in VA healthcare after the media exposure, with different patterns over time for women and men. Among women, levels of distrust increased in the first 90 days following media broadcasts regarding the scandal, followed by a significant decrease in distrust in days 90-180 post-media exposure. Among men, increases in distrust in the first 90 days following the media exposure did not reach statistical significance. Combined, our findings illustrate that well-publicized negative events can have measurable impacts on Veteran trust in the VA system, which could impact their willingness to receive care. This experience with evaluating rapid system change points to the importance of having tools in place to meet the challenges of the pandemic. No office is better placed than the VEO to accomplish this. In response to the pandemic, VA care changed dramatically in a matter of weeks. Whether patients with canceled appointments feel abandoned by their healthcare system needs to be ascertained. Also, understanding Veterans’ experience, satisfaction, and trust with telehealth is critical as our older, rural Veterans may be uniquely impacted by a digital divide. This is especially important as telehealth may largely replace routine face-to-face communication even after the pandemic. VEO’s journey maps can be designed to capture key bright spots and pain points in areas most important to Veterans during this pandemic, particularly in the telehealth journey experience. Capturing input from both Veterans and VA employees who may fear for their safety can provide further clarity into optimal care approaches during a pandemic. The journey of a COVID-19 hospitalized patient will differ from that of a non-infected patient needing an in-person procedure, as well as from the journey of a patient receiving care virtually. As a Health Services Research and Development (HSR&D) community, partnering with the VEO will help us to answer essential research questions such as: Which Veterans are at risk of losing trust in VA during the COVID-19 pandemic? What impact do social determinants of health play in the COVID-19 experience of care? How might the SHEP be revised to capture the exigencies of the moment? What qualitative questions should be asked to best capture the needs of Veterans and caregivers? With a strong VEO/HSR&D partnership, the innovation that our investigators bring can further the important goals of the VEO. 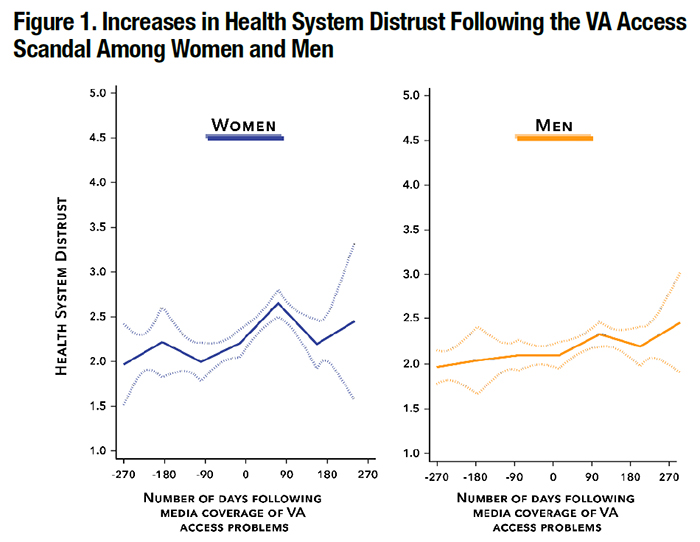
References
|
|